Depression and Memory Loss: How Depression Affects Your Memory?
Depression does more than change your mood. It can make it genuinely hard to remember things, stay focused, or think clearly.
Research consistently shows that depression causes measurable deficits in memory, attention, and processing speed, with some studies finding these problems persist even after mood improves.
This article explains what the science says, what kinds of memory problems depression causes, and what you can do about it.
How Depression and Memory Loss Are Connected?
Depression is not just a feeling. It changes how your brain processes and stores information. Multiple systematic reviews confirm that people with major depressive disorder show measurable deficits in attention, working memory, executive function, and processing speed.
These are not minor inconveniences. Effect sizes in meta-analyses range from about 0.34 to 0.65, which is large enough to affect daily life in real ways.
One of the most important things to understand is that memory problems in depression often start before you ever try to remember something. If your attention is poor at the moment you experience an event, that information never gets properly encoded.
Later, when you try to recall it, the memory seems weak or absent. This is why depression-related forgetfulness often feels like short-term memory loss, even when the core storage system is not severely damaged.
A large randomized study of 1,008 patients treated with antidepressants found that deficits in attention, verbal memory, response inhibition, and processing speed did not improve significantly after eight weeks of treatment, even in patients whose mood had remitted.
That finding matters because it shows cognitive symptoms can outlast the emotional ones.
What Types of Memory Does Depression Affect?
Depression does not hit memory in one uniform way. It tends to affect several overlapping systems.
Working Memory and Short-Term Recall
Working memory is your ability to hold information in mind while you use it. Think of following a recipe, tracking a conversation, or remembering a phone number long enough to dial it.
Depression consistently impairs this system. People often describe it as feeling like their mind goes blank mid-sentence, or like they read a paragraph and immediately forget what it said.
This is not imagined. A 2023 systematic review of neurocognitive deficits in depression found strong support for working memory impairment in both the acute phase of depression and in remission.
The problem tends to be worse during active episodes but does not always fully resolve when mood improves.
Episodic Memory
Episodic memory is your ability to recall specific events you have personally experienced. Depression impairs this too.
A meta-analytic review of episodic memory across the adult lifespan found that depression consistently weakens the encoding and retrieval of personally experienced events, including neutral ones that have no emotional charge.
Neuroimaging research helps explain why. A study of 46 participants found that depressed patients showed decreased activation in the right prefrontal cortex and right cingulate cortex during memory encoding, and disrupted coupling between hippocampal activation and later memory performance.
Healthy controls showed a strong link between medial temporal lobe activity and later recall. Depressed patients did not. This suggests the brain is not properly binding the details of events at the moment they happen.
Autobiographical Memory
One of the most replicated findings in depression research is something called overgeneral autobiographical memory. Instead of retrieving a specific event, people with depression tend to recall vague categories or repeated themes.
Ask someone without depression for a happy memory and they might say, “The dinner I had with my sister after her graduation last June.” Ask someone with depression and they might say, “Family events are usually bittersweet.”
A 2015 meta-analysis confirmed this pattern with a large effect size, particularly for positive cues. Depressed individuals are especially likely to fail to retrieve specific positive memories.
This matters because specific autobiographical memories support problem solving, future planning, and emotional regulation. When memory becomes vague and generalized, it can reinforce hopelessness and make it harder to draw on past successes.
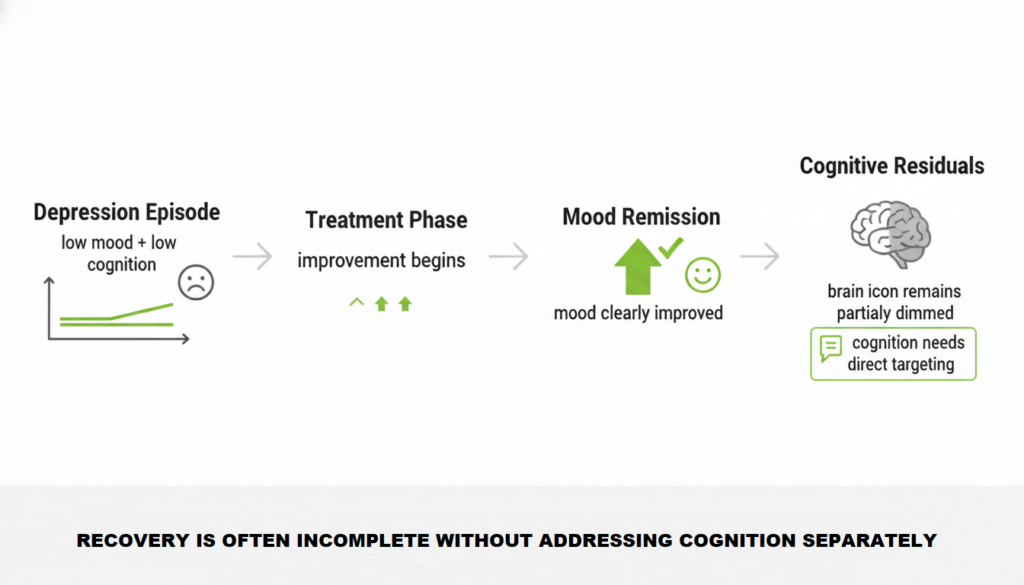
Why Memory Problems Can Persist After Depression Lifts?
Many people expect that once their mood improves, their thinking will sharpen too. The research suggests this is often not the case.
A large meta-analysis of 252 studies including nearly 12,000 remitted patients found significant cognitive deficits in 73 percent of the variables tested after remission.
Deficits in selective attention, working memory, and long-term memory persisted and worsened with repeated depressive episodes. The authors concluded that cognitive impairment in depression is at least partly independent of current mood state.
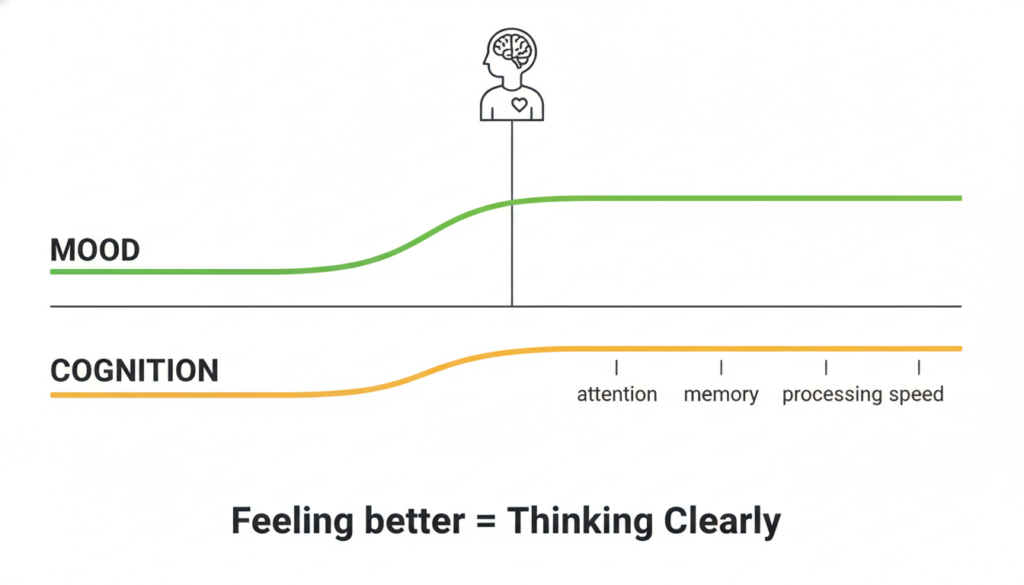
This is why some researchers now argue for “cognitive remission” as a separate treatment goal, distinct from mood remission. Feeling better emotionally does not automatically mean thinking clearly again.
Residual cognitive symptoms also matter because they raise the risk of depression coming back. Signs of depression relapse often include a return of concentration problems, forgetfulness, and mental slowing before the full emotional weight of a new episode sets in.
Recognizing these signs of depression coming back early gives you a better chance of getting support before things worsen.
Depression Relapse and Cognitive Warning Signs
Understanding depression relapse symptoms means paying attention to more than just mood. Cognitive changes are often among the earliest signs depression is coming back. You might notice:
- Trouble following conversations or losing your train of thought more often
- Forgetting recent plans, appointments, or what you just read
- Slower decision-making or feeling mentally foggy
- Difficulty organizing tasks that used to feel routine
- A return of that sense that your mind is not working the way it should
These signs of depression relapse can appear before low mood becomes obvious. A 2024 longitudinal study on residual symptoms in depression found that cognitive symptoms are among the most functionally consequential problems that remain after an episode and that they increase the likelihood of recurrence.
Treating them directly, rather than waiting for mood to worsen, is increasingly seen as important.
Can Depression Be Mistaken for Dementia?
In older adults especially, severe depression can produce cognitive symptoms dramatic enough to resemble dementia.
This is sometimes called depressive cognitive disorder, or historically “pseudodementia.” Clinical reviews describe presentations that include poor short-term recall, slowed thinking, attention problems, and apparent disorganization.
The distinction matters because the two conditions call for different responses. Some features that point toward depression rather than dementia include a more sudden onset, strong distress about cognitive symptoms, prominent low mood, and a history of previous depressive episodes.
People with early dementia often minimize their deficits; people with depression tend to amplify them.
That said, the picture is not always clean. A follow-up study found that older adults with depressive cognitive disorder had nearly four times the risk of later developing dementia compared with depressed older adults without cognitive impairment.
Depression can mimic dementia, but it can also precede it. This is why persistent or worsening cognitive symptoms in older adults deserve formal evaluation rather than reassurance alone.
The American Psychological Association’s updated guidelines on dementia evaluation emphasize that mood and cognitive symptoms must be assessed together, not in separate silos.
Depression, anxiety, ADHD, sleep apnea, and medical conditions like thyroid dysfunction or vitamin B12 deficiency can all produce overlapping cognitive complaints.
Does Treating Depression Fix the Memory Problems?
Partially, and sometimes not fully. Antidepressants can improve some cognitive domains, but the evidence is mixed. The large 1,008-patient study mentioned earlier found no significant improvement in five key cognitive domains after eight weeks of antidepressant treatment, even among those whose depression remitted.
A systematic review of pharmacotherapy in major depressive disorder found modest improvements in verbal memory, working memory, and processing speed across some studies, but executive function improved significantly in only two monotherapy studies.
Psychotherapy shows promise too. Cognitive behavioral therapy may reduce subjective cognitive symptoms and improve some domains.
A 2023 meta-analysis of cognitive rehabilitation in adults with major depressive disorder found moderate significant effects on executive function and verbal learning, and a significant effect on working memory.
This suggests that directly targeting cognitive symptoms, rather than assuming mood treatment will fix them, may be necessary for some people.
The practical takeaway is this: if you have treated your depression and your mood has improved but your memory and concentration still feel off, that is a real and recognized clinical problem. It deserves attention in its own right.
When to Seek Help?
Memory problems linked to depression are not a sign of weakness or imagination. They reflect real changes in how the brain encodes, stores, and retrieves information. You should consider speaking with a professional if you notice:
- Persistent forgetfulness that affects work, relationships, or daily tasks
- Cognitive symptoms that remain after your mood has improved
- Signs of depression coming back, including mental fog or slowed thinking
- Memory complaints that are worsening rather than staying stable
- Cognitive difficulties that feel disproportionate to your current mood
Getting a proper evaluation can help clarify whether what you are experiencing reflects depression, a co-occurring condition, medication effects, or something else entirely. Early support tends to lead to better outcomes.
If you are noticing signs of depression relapse or struggling with memory and concentration alongside your mental health, speaking with a therapist who understands depression can make a real difference.
Reach out to our team at Summit Wellness Group to learn how our depression treatment programs can help you move forward.


