Nutrition and Depression: Foods That Help Depression
Depression affects millions of people, and while food is not a cure, the evidence is clear that what you eat can meaningfully influence your mood.
Research now shows that people who follow a Mediterranean-style diet have a measurably lower risk of developing depressive symptoms over time.
This article walks you through the foods most consistently linked to better mood support, explains why they work, and shows you what to cut back on too.
Foods That Help Depression: What the Evidence Says?
The most important finding from recent research is not about a single “antidepressant food.” It is about the overall quality of your diet.
An umbrella review published in *Translational Psychiatry* found moderate-quality evidence linking higher adherence to healthy dietary patterns with lower depression risk.
A separate systematic review of 104 studies confirmed that the Mediterranean diet was associated with reduced depressive symptoms, lower stress, and better quality of life across diverse populations.
That means the best food strategy for depression is not a supplement. It is a shift toward eating more real, minimally processed food every day.
Why Dietary Patterns Matter More Than Single Nutrients?
It is tempting to look for one magic ingredient, but the science does not support that approach. What the research does support is that the combination of foods you eat regularly shapes your biology in ways that either protect or undermine your mental health.
Healthy diets appear to help mood through several overlapping pathways:
- Reducing chronic inflammation, which is repeatedly linked to depression
- Supporting a healthier gut microbiome, which communicates with the brain through the gut-brain axis
- Providing fiber that feeds beneficial gut bacteria and produces short-chain fatty acids
- Stabilizing blood sugar and reducing glycemic swings
- Supplying key nutrients like omega-3 fatty acids, zinc, folate, and magnesium
- Lowering oxidative stress and supporting neuroplasticity
A 2025 review titled *The Immune Mind* summarized this well, noting that Mediterranean-style interventions show moderate-quality evidence for reducing depressive symptoms in both major depressive disorder and subthreshold depression.
The mechanisms it highlights include anti-inflammatory effects, gut microbiota modulation, and changes in how the body processes stress hormones.
No single pill replicates all of that at once. Food does.
The Mediterranean Diet: The Strongest Food Pattern for Mood
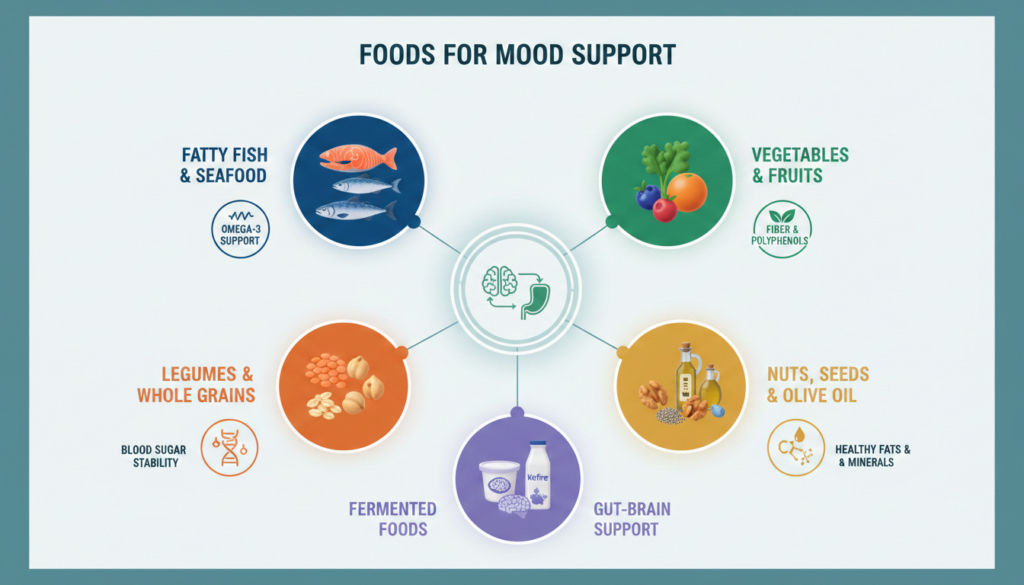
Among all dietary approaches studied, the Mediterranean diet has the broadest and most consistent support for mood benefits. It is not a rigid meal plan. It is a way of eating built around:
- Vegetables and fruits
- Legumes like lentils, chickpeas, and beans
- Whole grains
- Nuts and seeds
- Olive oil as the main fat
- Fish and seafood several times a week
- Lower intake of processed foods, red meat, and sugary drinks
A long-term community study found that older adults with greater adherence to a Mediterranean-based dietary pattern were less likely to develop depressive symptoms over 7.2 years, even after adjusting for health status, medications, and lifestyle factors. That kind of prospective evidence is meaningful because it tracks real people over real time.
The landmark SMILES trial, one of the most cited randomized controlled trials in nutritional psychiatry, showed that structured dietary improvement produced clinically meaningful reductions in depressive symptoms compared to a social support control condition.
Later trials in young men and in patients recovering from depression reinforced those findings.
The Best Foods That Help Depression and Stress
Fish and Seafood
Fish is the single food with the clearest and most repeated favorable signal in the depression literature. The *Translational Psychiatry* umbrella review found moderate-quality evidence for an inverse association between fish intake and depression risk.
Fatty fish like salmon, sardines, mackerel, herring, and trout are rich in EPA and DHA, the long-chain omega-3 fatty acids most relevant to brain health.
The key nuance here is that eating fish as part of a healthy diet is better supported than taking fish oil capsules for everyone.
A review on omega-3 fatty acids and depression found that supplements may help people with low baseline omega-3 levels, particularly as an adjunct to treatment, but they are not recommended as a universal prevention strategy. The food comes first.
For people who do not eat fish, plant-based ALA sources like flaxseed, chia seeds, and walnuts provide some omega-3s, though conversion to EPA and DHA is limited.
Vegetables and Fruits
Vegetables and fruits appear in every dietary pattern consistently linked to lower depression risk. They are not flashy, but they are foundational.
Research in adolescents found that each 100 g increase in daily fruit and vegetable consumption correlated with a 3% to 5% reduced risk of depression across multiple study designs.
Their likely contributions include fiber, folate, vitamin C, potassium, magnesium, and polyphenols. They also help by replacing less healthy foods in the diet, which matters just as much as what they add.
Legumes and Whole Grains
Legumes like lentils, black beans, and chickpeas supply fiber, folate, magnesium, iron, and plant protein.
Whole grains provide B vitamins, fiber, and steadier glucose regulation compared to refined carbohydrates. Both food groups are central to Mediterranean and plant-forward diets repeatedly associated with better mood outcomes.
They also feed the gut microbiome. A 2025 Frontiers review on gut microbiota and depression emphasized that healthy dietary patterns outperform single-nutrient supplementation partly because of synergistic effects on gut bacteria, short-chain fatty acid production, and inflammation control.
Nuts, Seeds, and Olive Oil
Nuts and seeds contribute healthy fats, zinc, magnesium, and vitamin E. Olive oil is a signature component of the Mediterranean diet and provides monounsaturated fats and polyphenols with anti-inflammatory properties.
Neither is a standalone treatment, but both help build the kind of dietary pattern that the evidence consistently supports.
Fermented Foods
Yogurt, kefir, and other fermented foods are increasingly relevant to mood research through the gut-brain axis.
A 2025 review found that psychobiotic and prebiotic approaches produce small-to-moderate improvements in depressive symptoms, particularly with multi-strain interventions lasting at least eight weeks.
Fermented foods are best seen as a supportive addition to a high-quality diet rather than a primary treatment.
Foods That Help With Depression and Anxiety: What to Reduce?
Knowing what to eat more of is only half the picture. The evidence on what to eat less of is equally strong.
Ultra-Processed Foods
This is the most consistent negative finding in recent nutritional psychiatry research.
A systematic review and meta-analysis found that high ultra-processed food consumption was associated with an odds ratio of 1.44 for depressive symptoms and 1.48 for anxiety symptoms, with a hazard ratio of 1.22 for subsequent depression in prospective studies.
A 2025 scoping review found that top-quartile ultra-processed food intake was linked with 25% to 40% higher risk of depression and anxiety, often in a dose-dependent pattern.
Ultra-processed foods include packaged snacks, sugary cereals, soft drinks, fast food, confectionery, and many ready meals. They are linked to worse mood outcomes through dysbiosis, inflammation, glycemic instability, and disruption of the gut-brain axis.
Reducing ultra-processed food intake may be at least as important as adding any single healthy food.
Sugar-Sweetened Beverages
The *Translational Psychiatry* umbrella review found moderate-quality evidence for a positive association between sugary drink intake and depression risk.
Swapping soft drinks for water, herbal tea, or coffee is one of the more straightforward dietary changes with mood-relevant support.
A Simple Guide to Mood-Supportive Eating
| Food Group | Examples | Why It Matters |
|---|---|---|
| Vegetables | Leafy greens, peppers, tomatoes, broccoli | Fiber, folate, polyphenols, antioxidants |
| Fruits | Berries, citrus, apples, bananas | Vitamins, fiber, anti-inflammatory compounds |
| Legumes | Lentils, chickpeas, black beans | Fiber, folate, magnesium, plant protein |
| Whole grains | Oats, brown rice, quinoa, whole grain bread | B vitamins, fiber, glycemic stability |
| Fish | Salmon, sardines, mackerel, herring | EPA and DHA omega-3s, anti-inflammatory |
| Nuts and seeds | Walnuts, almonds, flaxseed, chia | Healthy fats, zinc, magnesium |
| Olive oil | Extra virgin olive oil | Monounsaturated fats, polyphenols |
| Fermented foods | Yogurt, kefir | Gut microbiome support |
| Reduce | Soft drinks, packaged snacks, fast food | Linked to higher depression and anxiety risk |
Foods That Help Fight Depression: Key Nutrients to Know
While whole dietary patterns matter most, a few nutrients deserve specific attention because they appear repeatedly in the depression research.
Omega-3 fatty acids have the strongest individual nutrient evidence, particularly EPA and DHA from marine sources. They are best obtained through fish, but supplements may help as an adjunct in people with diagnosed depression and low baseline intake.
Zinc is one of the more underappreciated signals in the research. The umbrella review found moderate-quality evidence linking dietary zinc intake to lower depression risk. Good food sources include shellfish, meat, legumes, nuts, seeds, and whole grains.
Folate and B vitamins are found in leafy greens, legumes, citrus, and whole grains. They are biologically important for mood, and folate-rich foods are worth emphasizing as part of a healthy diet. People eating fully plant-based diets need to pay particular attention to vitamin B12, which is found mainly in animal foods or fortified products.
Magnesium is found in nuts, seeds, legumes, leafy greens, and whole grains. Ensuring adequate intake through food is sensible, though the evidence for magnesium supplements as a broad antidepressant is mixed.
Vitamin D is worth correcting if you are deficient, but its reputation as a mood supplement is stronger than the evidence supports. Large randomized trials have not consistently shown that vitamin D supplementation reduces depression risk in the general population.
The broader lesson is that getting these nutrients through food, as part of a high-quality dietary pattern, is more reliably supported than chasing them through supplements.

What Does This Mean in Practice?
You do not need a perfect diet to start seeing benefits. The research suggests that meaningful improvements in dietary quality can shift mood outcomes over time.
A practical starting point might look like this:
- Build meals around vegetables, legumes, and whole grains
- Add fatty fish two or three times a week if you eat it
- Use olive oil as your main cooking fat
- Include a handful of nuts or seeds daily
- Add yogurt or another fermented food where it fits
- Cut back on packaged snacks, soft drinks, and fast food
- Drink water or coffee rather than sugary drinks
For people eating fully plant-based diets, the evidence suggests real mood benefits are possible, but only when the diet is high quality and nutrient-adequate.
Poorly planned plant-based diets that are high in ultra-processed foods or low in B12 and iron may not offer the same protection.
Diet is One Part of a Larger Picture!
Food can support mental health in meaningful ways, but it works best alongside other evidence-based approaches.
Depression, anxiety, and chronic stress are complex conditions that often need professional support, therapy, and sometimes medication. Diet is a powerful adjunct, not a replacement for care.
If you or someone you care about is struggling with depression or a co-occurring mental health condition, speaking with a professional is an important step.
The Summit Wellness Group offers treatment programs that integrate nutritional support alongside evidence-based therapies for depression, anxiety, and related conditions. So, reach out to us today!