Stages of Anxiety: Levels, Anxiety Attacks Levels & Recovery
Anxiety can feel like a moving target. One day you might notice mild worry that fades by evening, and the next you’re gripped by intense fear that peaks within minutes.
Understanding the stages of anxiety, from minimal symptoms through moderate and severe levels, helps you recognize where you are and what kind of support will make the biggest difference.
Research shows that about 1 in 6 U.S. adults reported anxiety symptoms in a two-week period in 2019, with severity ranging from mild to severe.
This article explains the different stages of anxiety, the levels of an anxiety attack, and the evidence-based steps that guide recovery.
What Are the Stages of Anxiety?
Anxiety exists on a continuum. The Generalized Anxiety Disorder–7 (GAD-7) scale provides a widely used framework that divides anxiety into four severity bands: minimal (0–4), mild (5–9), moderate (10–14), and severe (15–21). These bands are not just labels. They reflect symptom load, functional burden, and the intensity of care you need.
The GAD-7 asks about seven core anxiety symptoms over the past two weeks, including nervousness, uncontrollable worry, excessive worry, trouble relaxing, restlessness, irritability, and feeling afraid as if something awful might happen.
Each item is scored from 0 (not at all) to 3 (nearly every day). Your total score determines your severity band and helps clinicians decide whether you need psychoeducation, therapy, medication, or a combination.
In primary care validation studies, a GAD-7 score of 10 or higher yields high sensitivity and specificity for DSM-based generalized anxiety disorder.
The scale also shows moderate accuracy in detecting panic disorder, social anxiety disorder, and PTSD, making it a practical general anxiety screener.
Different Stages of Anxiety: Minimal to Severe
Minimal Anxiety (0–4)
At this level, anxiety symptoms are absent or barely noticeable. You might feel occasional worry, but it does not interfere with daily life.
Most people in this band do not require treatment beyond general stress management and preventive education. If risk factors increase, such as a major life change or new health diagnosis, rescreening is appropriate.
Mild Anxiety (5–9)
Mild anxiety is the most common symptomatic level. In 2019, about 9.5% of U.S. adults reported mild anxiety symptoms.
You may notice persistent worry, restlessness, or trouble relaxing, but you can still manage work, social activities, and home responsibilities.
At this stage, psychoeducation and self-guided or brief guided cognitive behavioral therapy (CBT) are typically appropriate.
Monitoring every two to six weeks helps catch any escalation early. If symptoms persist beyond a few months, intensifying care is warranted.
Moderate Anxiety (10–14)
Moderate anxiety affects about 3.4% of U.S. adults in a two-week period. Symptoms are more frequent and harder to control.
Worry may interfere with concentration, sleep, and relationships. You might avoid certain situations or need reassurance more often.
This level calls for diagnostic evaluation and first-line treatment. Evidence-based psychotherapy, especially CBT or acceptance and commitment therapy (ACT), is effective.
First-line medications such as duloxetine, pregabalin, venlafaxine, or escitalopram may be considered based on your preference, comorbidities, and functional impairment. Monitoring every two to four weeks helps track progress and adjust treatment as needed.
Severe Anxiety (15–21)
Severe anxiety affects about 2.7% of U.S. adults in a two-week period. Symptoms are intense and pervasive. You may feel overwhelmed nearly every day, struggle to leave home, or experience physical symptoms like chest tightness, dizziness, or shortness of breath. Work, school, and relationships often suffer.
Combined treatment, psychotherapy plus pharmacotherapy, is frequently warranted at this stage. Safety and functional impairment should be addressed aggressively.
Close monitoring, initially every one to two weeks, helps ensure early response. If improvement stalls by four to six weeks, expedited specialty care or treatment augmentation is appropriate.
Are There Stages of Anxiety Attacks?
Yes. Anxiety attacks, more precisely called panic attacks, unfold in a predictable arc. A panic attack is an abrupt surge of intense fear or discomfort that peaks within minutes, accompanied by symptoms like palpitations, shortness of breath, dizziness, derealization, and fear of dying.
Research using ecological momentary assessment and ambulatory physiology reveals that panic attacks are not isolated spikes.
They are the peak of a dynamic process shaped by anticipatory anxiety, interoceptive appraisal, autonomic reactivity, and behavior. Understanding the stages of an anxiety attack helps you recognize early warning signs and apply coping strategies before symptoms peak.
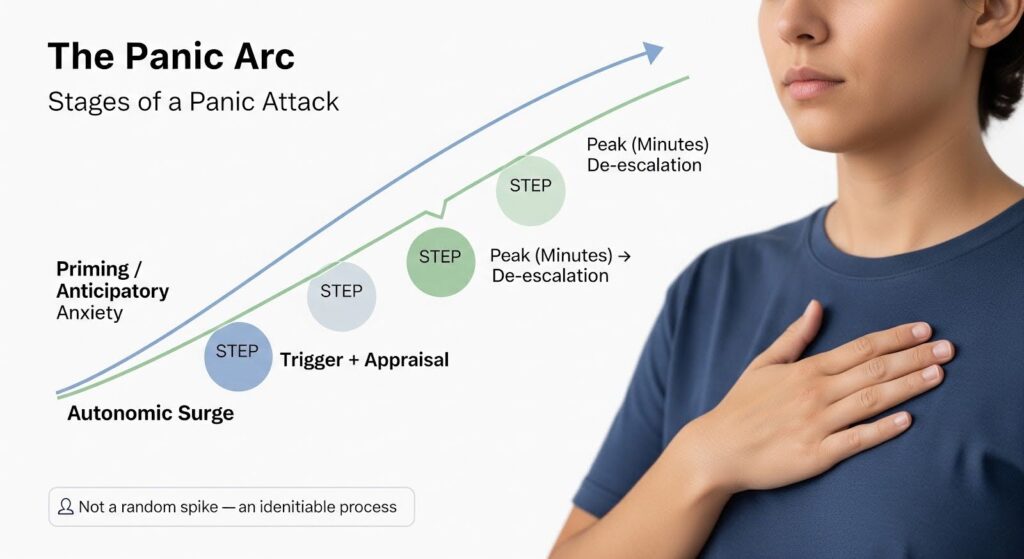
Stage 0: Vulnerability and Priming (Hours to Days Before)
Before an attack, you may notice heightened threat expectancy, rumination, and low coping self-efficacy. Diurnal anticipatory anxiety often increases at certain times of day or in specific contexts. Sleep disruption and stress can lower your threshold for panic. Subtle avoidance and scanning for bodily cues are common.
Resting heart rate variability (HRV) measured by consumer wearables may decline during vulnerable periods, particularly during sleep, though this is context-dependent and should not be overinterpreted.
Stage 1: Trigger Detection and Initial Appraisal (Seconds to Minutes)
A trigger, internal like caffeine or exertion, or external like a crowded space, sparks catastrophic misinterpretation of benign interoceptive cues.
For example, you might interpret normal tachycardia as a heart attack. Initial autonomic arousal and respiration changes begin. You may orient to escape routes or engage in micro-avoidance.
This is the teachable moment targeted by interoceptive exposure, a core ingredient in effective CBT. Interoceptive exposure deliberately elicits feared bodily sensations under controlled conditions to decouple sensation from catastrophic meaning.
Stage 2: Escalation and Autonomic Surge (Minutes)
Spiraling confirmation bias takes hold. You think, “I am losing control.” Sympathetic surge produces tachycardia, dyspnea, dizziness, and sharply reduced HRV.
Hyperventilation and escape attempts are common. Intensity ratings captured by ecological momentary assessment and ambulatory physiology peak during this stage.
Stage 3: Peak Panic (Peaks Within Minutes)
This is the apex. You feel a sense of imminent catastrophe, death, insanity, or loss of control. Arousal is maximal. Freeze or flight behaviors dominate. High-distress verbalizations and clinical observations confirm the peak.
Stage 4: De-escalation (10 to 60 Minutes)
Gradual reappraisal begins. Parasympathetic rebound brings fatigue and trembling. You may rest, seek reassurance, or cling to safety behaviors. HRV begins to normalize during rest or sleep. Residual worry about recurrence persists.
Stage 5: Aftermath and Consolidation (Hours to Days)
Memory reconsolidation and meaning-making occur. Without corrective learning, avoidance generalizes and anticipatory anxiety strengthens. Perceived coping self-efficacy moderates how much anticipatory anxiety increases after an attack.
Weekly measures like the Panic Disorder Severity Scale—Self-Report (PDSS-SR) capture anticipatory anxiety, avoidance, and role impairment during this stage.
Anxiety Level and Recovery: What Works at Each Stage?
Recovery is not a single event. It unfolds across three horizons: acute stabilization, subacute symptom reduction, and long-term relapse prevention.
Acute Recovery (Hours to Days)
Physiological normalization, immediate coping, and safety planning are priorities. If you present to an emergency department during a peak panic episode, medical evaluation rules out cardiac or respiratory causes. Rapid education, reassurance, and referral to stepped-care panic interventions reduce recurrent emergency visits.
Subacute Recovery (Weeks)
Symptom reduction through evidence-based psychotherapy is central. CBT with interoceptive and in vivo exposure is the most empirically supported treatment for panic disorder. Protocols that include interoceptive exposure are consistently superior to those that omit it for panic frequency and global severity outcomes.
Interoceptive exposure counterconditions catastrophic beliefs by pairing feared bodily sensations, dyspnea, palpitations, with safety learning. This reduces avoidance and anticipatory anxiety.
A recent randomized controlled trial found that brief intermittent intense exercise (BIE) can serve as interoceptive exposure with durable benefits.
Participants who engaged in BIE had fewer and less severe panic attacks and better depressive symptom outcomes at six months compared to relaxation training. Patients reported BIE as more enjoyable, suggesting better engagement. BIE operationalizes interoceptive exposure at scale, low-cost, health-promoting, and naturally extendable into daily life.
Where indicated, first-line pharmacotherapies such as duloxetine, venlafaxine, escitalopram, or pregabalin may be combined with CBT.
Benzodiazepines are superior to placebo for rapid symptom control, but dependence risk justifies cautious, time-limited use as a bridge while CBT and SSRIs take effect. Avoid benzodiazepines in patients with substance use risk and in most older adults.
Digital CBT programs that embed interoceptive exposure, inhibitory learning strategies, and personalization can approach traditional CBT efficacy, especially when access to face-to-face therapy is limited.
Self-guided virtual reality CBT shows short-term promise and autonomic improvement but currently lags conventional, interoceptive-heavy CBT in component-level efficacy.
Maintenance and Relapse Prevention (Months to Years)
Generalization of gains into daily life and durable behavior change are the goals. Continued interoceptive and situational exposures, including BIE as “lifestyle interoceptive exposure”, help prevent the reemergence of vulnerability and priming cycles.
Patients who enjoy BIE are more likely to maintain engagement, sustaining autonomic and cognitive resilience.
Measurement-informed care is essential. Weekly PDSS-SR, periodic functional assessments using the WHO Disability Assessment Schedule 2.0 (WHODAS 2.0) or Sheehan Disability Scale, and appropriately interpreted resting HRV summaries form a robust monitoring suite.
These tools detect early signs of relapse, rising anticipatory anxiety, widening avoidance, declining function, and trigger booster exposures or medication adjustments.
What is Mild Anxiety vs. Moderate Anxiety?
The distinction between mild and moderate anxiety is both quantitative and functional. Mild anxiety (GAD-7 5–9) involves noticeable symptoms that do not significantly interfere with daily roles.
You can still work, socialize, and manage home responsibilities, though you may feel more effort is required.
Moderate anxiety (GAD-7 10–14) crosses a threshold where symptoms interfere with concentration, sleep, and relationships. You may avoid certain situations or need frequent reassurance.
This level warrants diagnostic evaluation and first-line treatment, psychotherapy, pharmacotherapy, or both, with monitoring every two to four weeks.
The GAD-7 does not explicitly assess some DSM-5 domains like difficulty concentrating, sleep disturbance, and functional impairment.
For both diagnostic and staging accuracy, especially at moderate and severe levels, the GAD-7 should be supplemented with functional impairment queries, sleep and concentration items, and DSM-5-TR disorder-specific severity measures when panic, social anxiety, or other syndromes are suspected.
Demographic Patterns and Health Equity
Anxiety severity varies by sex, age, and race/ethnicity. Women consistently report higher GAD-7 symptom severity. Severity decreases with age.
In 2019, non-Hispanic White adults were most likely and non-Hispanic Asian adults least likely to report mild, moderate, or severe symptoms.
These differences may reflect true prevalence variation, cultural expression of distress, stigma, access, and measurement artifacts.
Measurement invariance across gender and age is supported, but ongoing evaluation in U.S. racial and ethnic subgroups is prudent. Tailoring outreach and ensuring linguistically and culturally validated instruments is essential.
Longitudinal Dynamics: How People Move Between Stages?
Anxiety severity is dynamic. A multi-state Markov model applied to a coronary heart disease cohort found that 84 to 87% of those with no baseline anxiety remained asymptomatic over five years.
About half with mild anxiety transitioned to no symptoms, and roughly one-third with moderate to severe anxiety remitted. Yet a substantial subset persisted, validating repeated measurement and stepped escalation when scores remain in moderate or severe bands.
Trajectory modeling during antidepressant treatment underscores heterogeneity in response. Early nonresponse at moderate or severe levels should trigger augmentation or modality changes. Weekly to monthly GAD-7 staging steers treatment pathways in real time.
Special Considerations for Older Adults
Older adults require tailored assessment and cautious pharmacotherapy. The 2024 Canadian guidelines for anxiety in older adults emphasize slower titration, avoidance or minimization of benzodiazepines due to fall risk, cognitive impairment, and dependence.
Behavioral interventions remain central, with careful attention to medical comorbidities and sensory or cognitive barriers to exposure work. Functional targets like WHODAS or the Sheehan Disability Scale may be particularly salient markers of recovery in this population.
A Practical Staging Framework
Adopt a dual-threshold GAD-7 policy: use 10 or higher to initiate diagnostic evaluation and treatment planning; use 8 or higher as a triage threshold in primary care to minimize missed cases, with a requirement for confirmatory assessment pathways.
Where robust local validation exists, such as in epilepsy, where a GAD-7 cutoff greater than 6 maximized diagnostic accuracy, recalibrate thresholds to maximize diagnostic accuracy.
Supplement the GAD-7 with DSM-5-TR disorder-specific severity measures and function, sleep, and concentration probes at moderate to severe levels or when syndrome differentiation guides treatment selection.
Deploy a stepped-care ladder tied to severity and trajectory: mild, brief or guided psychotherapies with monitoring; moderate, psychotherapy and/or first-line pharmacotherapy; severe, combined therapy, short-interval follow-up, and rapid escalation if early nonresponse.
Institutionalize repeated measurement: weekly to monthly GAD-7 during acute treatment; monthly during maintenance; apply pre-specified change thresholds to trigger augmentation or switch strategies.
Integrate digital care to close gaps: guided internet-based CBT, phone psychotherapy, and measurement-based care dashboards embedded in electronic health records can expand access, maintain fidelity, and support equity by delivering intensity matched to stage.
Why Understanding Stages Matters?
Understanding the stages of anxiety, from minimal through mild, moderate, and severe, empowers you to seek the right care at the right time.
Recognizing the stages of an anxiety attack helps you apply coping strategies before symptoms peak and engage in corrective learning afterward. Recovery is a process that unfolds across acute stabilization, subacute symptom reduction, and long-term relapse prevention.
The strongest evidence supports a stage-based, exposure-centric approach anchored in interoceptive and situational exposure, enriched with brief intermittent intense exercise where suitable, selective use of SSRIs or SNRIs, and weekly measurement with the PDSS-SR and functional scales.
Digital tools like ecological momentary assessment and wearables add value when used judiciously to personalize triggers, detect early drift, and provide motivating feedback on autonomic flexibility improvements.
If you or someone you care about is navigating anxiety at any stage, compassionate, evidence-based support can make all the difference. Reach out to our team to explore personalized treatment options that meet you where you are.


